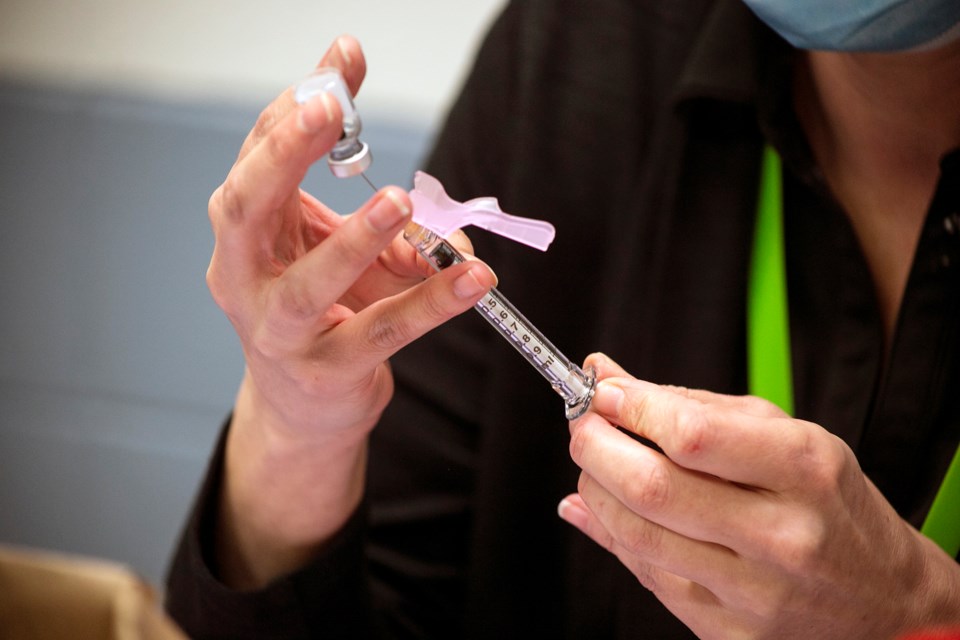
Will Canadians still be lining up at vaccine clinics post pandemic if they need booster shots for COVID while risks for the virus seem low?
University of Guelph history professor Catherine Carstairs says we could learn a thing or two from past epidemics.
Carstairs said that when she and graduate student Curtis Fraser studied polio and H1N1 outbreaks in the past, they found that people are eager to get vaccinated when the disease seems to be a risk to themselves and their families. But when the risk seems to drop, people are less inclined to get the vaccine which could become problematic.
She gives the example of the polio epidemic.
“Polio was terrifying for parents in the early 1950s, the children ended up paralyzed from polio and sometimes ended up with iron lungs which were the artificial respirators of the time period,” she said, adding that parents were eager to get their children vaccinated when the vaccine came out in 1955.
She further explained that younger adults in their 20s and 30s didn’t get vaccinated because they didn’t perceive themselves to be at risk as polio was often called infantile paralysis and was generally associated with children despite it being a risk to all ages.
“So we saw subsequent polio epidemics in the late 1950s including quite a severe one in 1959 that had a bigger impact on young adults than it did on children,” said Carstairs.
“And that's because only about 10 per cent of young adults were vaccinated, so that's one of the challenges, persuading everybody that they're at risk of the disease.”
Carstairs said another discovery from the study of the polio epidemic is the fear of needles among many people. In the early 1960’s, the Sabin vaccine was introduced which was an oral vaccine.
“It was often served as a sugar cube and it was quite tasty and that seems to have encouraged people to take the vaccine as well, especially those who've been hesitant because they were scared of needles,” said Carstairs.
She said right now, people have been very eager to get the vaccine but now that COVID cases are dropping significantly, it is going to become harder to target the remaining population to get their first vaccine.
“They're not going to perceive it to be as risky as it obviously felt two months ago,” said Carstairs.
She said in learning from past epidemics, the vaccine needs to be accessible as much as possible.
“Some of these things (vaccine availability) have already happened and, and in some cases they can be expanded on so taking vaccines to work places, making sure that people don't have to travel long distances to get their vaccines,” she said adding that vaccines could be administered in schools, by family doctors etc. especially in rural places where it is more difficult to get the vaccine.
She also gives the example of the H1N1 virus that emerged in the spring of 2009. After a child in Toronto died, parents were frightened and began lining up at the vaccine clinics.
“There was immense enthusiasm for getting the vaccine but as it turns out, H1N1 was more mild than people had initially feared that it might be. And in the end, the uptake of the H1N1 vaccine was pretty similar to what we see with the yearly flu vaccine,” said Carstairs.
“I think with the flu vaccine, there's a lot of people who always feel like not that serious of a disease even though we know lots of Canadians die of the flu every year so I think a lot of people either think the flu isn't that serious or it won't be that serious for them.”
She said the biggest challenge public health authorities might face is ensuring the continued uptake of COVID vaccines once the initial crisis of this pandemic has passed.That will likely mean more measures to combat vaccine misinformation and measures to ensure that vaccines are readily available and convenient to access for the general population.